*Please note: This slide show represents a visual interpretation and is not intended to provide, nor substitute as, medical and/or clinical advice.
There is no cure for COPD, however, lifestyle changes and treatments can help you feel better, stay more active, and slow disease progression.
The goals of COPD treatment are to relieve symptoms, slow the progression of disease, improve exercise tolerance, prevent and manage complications such as “flare-ups”, and improve overall health.
Patients should become informed about COPD by speaking with their doctor. Sometimes a referral to a pulmonologist, or lung doctor, may be required. Patients who are informed about their COPD are likely to have better health outcomes.
COPD interventions may consist of lifestyle changes, medical treatments, vaccinations, oxygen therapy, and pulmonary rehabilitation. A small number of patients may also require selective surgical procedures.
Lifestyle changes are important. Quitting smoking is vitally important, and your doctor and support groups can help you quit. COPD risk increases with smoking, and ranges from 35% to as high as 50%.
Avoiding second hand smoke and other lung irritants like air pollution (dust and chemical fumes) is also very important.
Getting regular exercise may also greatly benefit persons with COPD.
Medical treatment of COPD may consist of inhaled medications and oral medications.
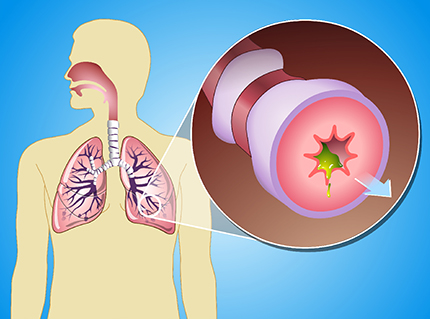
The most important medicines used to treat COPD include inhaled bronchodilators, which patients breathe in to the lungs to open up (or dilate) the airways (or bronchi); thus these medicines are called bronchodilators.
Other medicines can be used with the bronchodilators in special situations and include inhaled corticosteroids, oral methylxanthines (such as theophylline), or oral phosphodiesterase-4 inhibitors.
Bronchodilators relax the muscles around the airways, allowing the airways to open up more or dilate so that you can breathe better. Most bronchodilators are taken with inhalers, which allow the medication to go straight to your lungs. Using inhalers the right way is very important, and your healthcare provider or pharmacist can instruct you on their correct use.
Short-acting, or quick relief, bronchodilators can be prescribed as needed for trouble breathing. The long-acting bronchodilators are usually given to you if you have ongoing symptoms of COPD and should be taken regularly – whether or not you are having trouble breathing. The long-acting bronchodilators work better than the short-acting bronchodilators to help improve the long-term symptoms of COPD. But the long-acting inhalers are often more expensive than the short-acting inhalers.
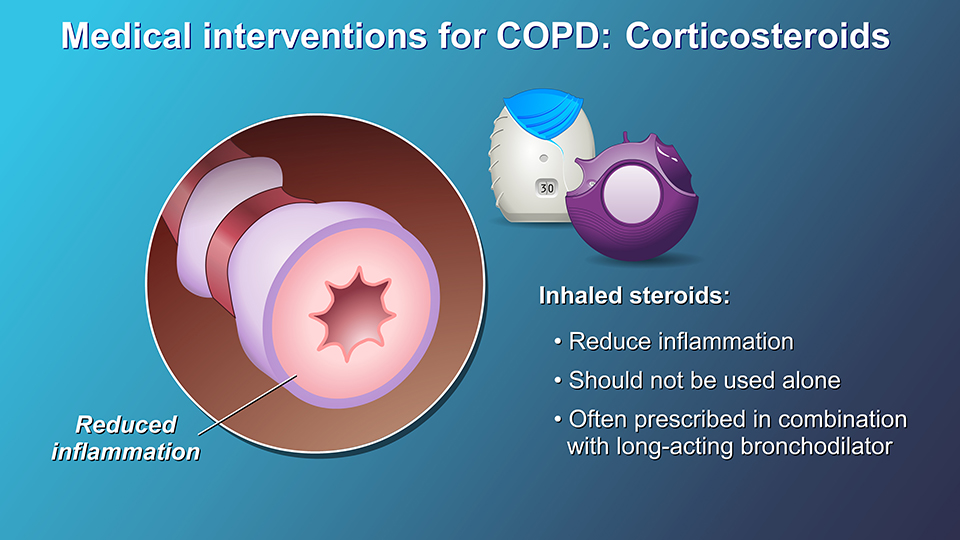
Inhaled corticosteroids are also used for the treatment of COPD. Inhaled steroids may help to reduce inflammation in the lungs. If your COPD becomes more severe, or if your symptoms flare up often, your doctor may prescribe a combination of a bronchodilator and an inhaled steroid.
Inhaled steroids should not be used alone, without also using a long-acting bronchodilator for COPD. Your doctor may want you to try this combination to see whether the addition of an inhaled steroid to a long-acting bronchodilator helps to relieve your symptoms and/or reduces your chances of having flare-ups (or exacerbations of COPD).
Another medical treatment for COPD is a class of drugs known as phosphodiesterase-4 inhibitors (or PDE-4 inhibitors).
If you don’t have relief of symptoms, or if your COPD exacerbations continue, your doctor may decide to prescribe a PDE-4 inhibitor to lower your chances of having more COPD exacerbations and improve your quality of life.
Antibiotics are also used to control bacterial lung infections in COPD, especially during acute flare-ups. These drugs treat sudden infections that may arise from time to time in the course of COPD.
Oral corticosteroids should only be used during acute flare-ups, or acute exacerbations of COPD, and should not be used on a routine basis. These medicines, when used during an acute exacerbation of COPD, help you get over the flare-up faster, reduce your chance of relapsing, and lower your chance of having to be admitted to the hospital.
Prevention of infection is very important in persons with COPD, who are at greater risk for complications from flu and pneumonia. Vaccines can help prevent illness and can help to lower chances of getting a flare-up and needing hospital care.
Oxygen therapy may be needed in persons with COPD. If you have severe COPD and your oxygen levels are lower than normal, the use of supplemental oxygen can help you breathe better and improve your physical activity. Oxygen has benefits to enable better sleep, provide greater exercise tolerance, and lower your chances of dying with COPD.
Pulmonary rehabilitation is recommended for most people with COPD.
Rehabilitation may include an exercise program, disease management training, as well as nutritional and psychological counselling.
The goal is to help persons with COPD to stay healthy, carry on with daily activities, follow healthy eating habits, sleep well, and better manage exacerbations of their illness.
In rare cases, surgical intervention may be recommended for persons with COPD who have severe symptoms that have not improved with medical therapy.
Lung-volume reduction (or LVR) surgery is the removal of damaged tissue from the lungs, helping to improve breathing and quality of life, but only helps a few, select people with COPD.
Lung transplantation involves replacing a damaged lung with a healthy lung from a donor. This surgery can improve your lung function and quality of life, but has many risks such as infections or rejection of the transplanted lung. Your doctor can discuss the benefits and risks of this surgical option with you.
Managing complications is very important for persons with COPD. The symptoms of COPD may worsen over time; however, they can also worsen suddenly if a cold or the flu occurs. Breathing may become difficult and you may experience chest tightness, increased coughing, your sputum may change color, and you may have a fever. Call your doctor right away should this happen.